
Humana Agent Resources and Materials

Humana’s Bonus Just Got Better for Q2 2024!
On top of the exciting $300 bonus for Underwritten Policies, we’re now adding a $300 bonus for each eligible Medicare Supplement Plan N Open Enrollment Policy. See details below.
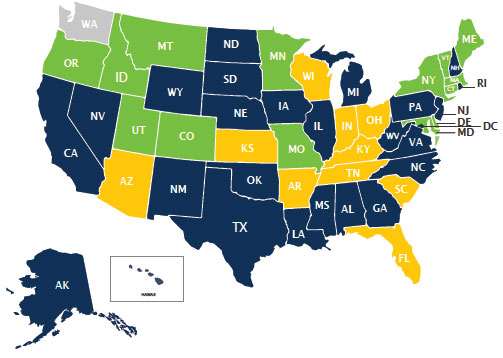
| $300 for Underwritten and Plan N Open Enrollment applications, $100 for other plan Open Enrollment applications |
| $300 for Underwritten/Open Enrollment applications |
| $100 for Underwritten/Open Enrollment applications |
View the Humana Achieve Q2 2024 Agent Incentive Flyer for full details.
2024 Individual Products Producer Partnership Plan
Humana MCA / HRA Updates
On September 1, Humana is transitioning from a standalone MCA survey to the HRA (Health Risk Assessment) and at the same time transitioning to a new survey platform.
On August 31st we will decommission the MCA survey on the Icario/Amplify platform, and turn on the HRA on the Sunfire platform.
The HRA is an optional, online, scripted survey that agents administer to new to Humana Medicare Advantage members. For SNP members, the HRA is a CMS requirement.
With this transition, all agents will need to take a CMS required Model of Care Training, (MOC). Humana has included this in the annual cert/recert. process.
- Cert/Recert launched June 27, 2023 ending on November 30, 2023
- Agents will need to complete MOC training by August 31, 2023 to administer the survey and have access to the Sunfire portal.
- Tools Training for the Sunfire platform will be available in HMU in August.
What you need to know:
- Transitioning from our current vendor Icario/Revel to Sunfire
- MCA will transition to the HRA (Health Risk Assessment)
- Agent has 30 days to complete the survey with the member
- Agent will receive incentive based on current payment structure by channel with new enrollment
- Member can still qualify for the Healthy Spending Card with the HRA survey
HRA will have approx. 20 questions - New additional languages have been added for survey administration
- All agents must complete the Model of Care training
- Agents will need to complete Cert/Recert no later than 8/31 to compliantly administer the HRA on 9/1
- To experience no gap in their ability to offer Humana’s health survey to members and remain eligible to earn the HRA admin fee
- Humana and Sunfire are launching the HRA on 9/1/23.
- Partners do not have to meet that timeline necessarily, but 9/1 would be the earliest that the link into Sunfire would be active for agents to access the HRA
PY2024 Certification Now Open!
PY2024 Cert/Recert is now open! Attached are some helpful guides for you and your colleagues.
This year, Humana is making a change to our Member Care Assessment program. We are moving to an HRA, and there is a new training required that is housed within PY2024 Cert/Recert. The new HRA is scheduled to roll out 9/1, so certifying by 8/31 is ideal so you will have acecss to the HRA program and be eligible for compensation. Below are additional details.
Member Care Assessment transition to Health Risk Assessment:
- As annual CMS requirement of those conducting HRA’s, the Model of Care (MOC) training will be rolled out to agents in the Humana Certification and Recertification training starting in PY24.
- Be on the lookout for the tool training (Health Care Assessment Training) on Sunfire after cert/resert opens
*** Please note that August 31, 2023 is simply the deadline for the 9/1 start date for HRA. If an agent completes training past 8/31/23 they will still be able to access the Sunfire portal to complete surveys and qualify for compensation as the current program guidelines indicate, we are just highlighting that date to be in line with the roll-out and ensure agents are aware that the training is required to be compensated.***
Accessing – Transferring AHIP Scores Job Aid
How to Complete Humana MAPD & PDP Certification & Recertification
Updated 2023 DSNP playbook
Learn the latest about DSNPs with our DSNP playbook including DSNP basics, verification, the deeming period and lead-generation info. Plus, explore a new section on the SNP Care Management and Health Risk Assessment.
Agent Notice of Updates to the 2023 PPP – 1/30/23
There has been a small change to our Commission Schedule.
This updated version of the 2023 PPP now contains two commission schedules for Achieve Medicare Supplement Products as outlined below:
- Applicable to policies with effective dates between January 1, 2023 and February 28, 2023″ (see pages 21 – 31).
- Applicable to policies with effective dates on or after March 1, 2023″ (see pages 32 – 40).
You can view the schedule at http://www.Humana.com/SellHumana.
The New Election Period Playbook
Navigating election periods just got easier. With Humana’s Election Period Playbook, you can find information for the Open Enrollment Period (OEP) and Special Election Periods all in one resource. Get the playbook to understand the ins and outs of selling outside of the Annual Election Period (AEP).
Humana Medicare Enrollment Job Aid (2023)
2023 Humana Playbook Final
Click below for the 2023 Humana MN and ND Playbook Final, including PDP information. In addition, is a copy of the Dental Highlights Grid for Minnesota and North Dakota. Soon, Humana will get the Dental “Slicks” out that will show exactly what procedures covered for each DEN plan built into our MA plans.
Reminder on Homework Items:
- Get savvy on at least one electronic method of enrollment w/ Humana Fast App or EHub
- Learn to use Digital Marketing Materials (On the Agent portal) send to yourself as a trial.
- Get ready to do Member Care Assessments, Free MONEY, $60 extra compensation per eligible assessment completed! MarketPOINT University (enter Member Care Assessment in the search bar) You will get email from Revel Connect to establish an account
- Register for Humana Reach Rewards-SO EASY! www.Humanareachrewards.com
Humana’s Medicare footprint is expanding in many states and counties in 2023
Humana is excited to share that our plan offerings continue to grow, and in AEP 2023 we will be expanding our Medicare plans across multiple categories in a number of new markets – growing our footprint to 1.59M total eligibles including 500K total Dual eligibles.
We are dedicated to enhancing the member experience by investing in plans and plan features that meet consume needs. These expansions are a significant development in our overall footprint offering:
- More choice for for the consumer
- Greater access to care
- Opportunity to improve health outcomes
Click below to to access an outline and familiarize yourself with the expanded plan offerings in your market starting AEP 2023.
CMS strictly prohibits dissemination of 2023 plan information before October 1, 2022.
2023 Sales Materials available for order this July!
New agent certification and recertification begins June 28th. Make sure to certify or recertify in order to get the most recent sales materials for this upcoming plan year. 2023 sales materials will be available to order beginning July 20th. If you certified/recertified prior to July 20th, you will receive an email with a product guide and the link to order sales materials, once they’re available.
How To Order Sales Materials
| You can order through the certification/recertification courses | |
| You can order through Vantage, under the ‘Medicare’ section by clicking the ‘Medicare Sales Materials’ link | |
| You can also order through the individual link provided here. |





